The pandemic made people face difficult problems in every aspect of their life. Medicine and healthcare were also kind of victims of the whole COVID-19 situation. However, in a press release, Phillips reveals which are the 10 technology trends which are on their way to taking over this year.
Freeing up focus for patient care by automating routine tasks with AI
Highly capable professionals spend an undue amount of time on routine tasks that pull their attention away from the patient. For example, in radiology departments, imaging staff say almost 25% of their work is inefficient and could be automated.
We now have the tools to automate such tasks to relieve the burden on imaging technologists and free up focus for patient care. AI-enabled technology can make it easier for technologists to plan and execute routine exams, helping them to get images first-time-right with enhanced confidence and precision.
We will see an increased use of AI-based automation in image-guided therapy, where physicians perform minimally invasive procedures on patients with heart disease or other conditions. Interventional physicians may spend up to two hours reporting on cases after a full day of treating patients. AI could help alleviate this workload by auto-logging different steps of the procedure – enabling physicians to give their full attention to providing patient care.
Improving access to care through virtual collaboration between providers
64% of global healthcare leaders say they’re currently investing heavily in virtual care. But while this healthcare technology trend is generally seen as impacting the patient-provider relationship, the rise of virtual collaboration between providers themselves offers equally promising opportunities.
The adoption of tele-ICUs in acute care is a prime example. A tele-ICU can extend critical care resources to the bedside, no matter where the hospital is.
By using a live collaboration platform, experienced sonographers can remotely assist their local counterparts with exams, while colleagues can use the same platform to discuss patients’ medical status with them.

Photo Credits: Philips
Connecting the hospital to the home with virtual care
Health technology innovations are enabling people to better engage with providers, access more care overall, and get the resources they need to stay informed while taking more preventative healthcare measures.
Healthcare providers are turning to remote patient monitoring and virtual visits in order to maximize access to care, strengthen connections with at-risk populations, minimize the risk of COVID-19 transmission, provide more convenient experiences and reduce the strain on scarce hospital resources.
According to the World Bank and World Health Organization (WHO), half the world still lacks access to quality care, and without drastic action, the WHO estimates that 5 billion people will be unable to access healthcare by 2030. World-leading healthcare organizations continue to pioneer digital health technologies that bring care closer to patients and partner with local providers to keep improving access to quality healthcare for everyone, no matter where they live.
Offering more services at facilities closer to patients
Another healthcare technology trend enabling more equitable access to care is the move from hospital-centric to locally delivered care. Patients who have traditionally had to travel long distances for state-of-the-art or specialized healthcare can access these technologies via smaller (and sometimes even mobile) healthcare facilities.
Out-of-hospital settings like local diagnostic hubs, Virtual Care Stations, and even technology-equipped container structures can offer closer-to-home healthcare that’s especially vital for people living in rural and underserved communities. Primary care facilities and local clinics, through a combination of virtual specialist support and technologies such as ultrasound and X-ray imaging, can now function as remote hospitals, providing services such as ultrasound exams to pregnant women. If a patient comes in with a broken wrist, a local practitioner can make an X-ray and immediately share it with a remote traumatologist, radiologist or emergency doctor for remote consultation instead of requiring the patient to make a lengthy trip to a big-city hospital.
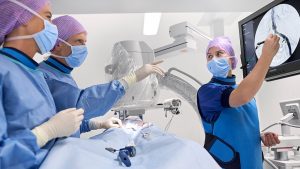
Photo Credits: Philips
Certain types of specialist treatment have also become more routine, giving rise to the growing trend of office-based labs and ambulatory surgery centers that offer patients access to potentially life-saving minimally invasive procedures closer to their communities.
In the near future, one can imagine nurses routinely performing ultrasound exams at retail or community centers, using a portable handheld device with support from a remote expert sonographer and AI algorithms that can extract basic information from the scan.
Integrating data to enable clinical collaboration and patient-centered care
Multidisciplinary care teams are trying their best to connect and keep track of all relevant information pertaining to their patients – from a variety of subspecialty reports to information about patients’ current condition, demographic data, and health history. Deciding on the right therapy is equally complex, especially in areas like oncology where physicians and patients may face a bewildering number of choices.
Integrated diagnostics is a rapidly evolving field where organizations have smart, connected systems in place that give them comprehensive and actionable insights into their patient populations by uniting imaging, monitoring, laboratory, genomics and longitudinal data. Multidisciplinary tumor boards are an example of this healthcare technology trend. With integrated diagnostics solutions, care teams can now deliver comprehensive, patient-centric cancer care, uniting patient data from disparate sources in dashboards, thus facilitating collaborative diagnostics, treatment and follow-up decisions.
Using predictive analytics to proactively manage transitions of care
Using the power of AI and predictive analytics, we can now extract relevant insights on patient flow and patient care needs from vast amounts of real-time and historical hospital data, to predict capacity needs in the next 24 to 48 hours. After initial validation, the resulting algorithms can be updated on a regular basis to take recent trends and circumstances into account – offering clinical and operational teams the real-time, actionable insights they need to make timely and effective decisions.
By embedding these data-driven practices into everyday management of patient flow, healthcare systems will be able to get the most out of precious resources and manage transitions of care more effectively across the patient journey, from hospital admission to discharge and back into the home – ensuring that the patient gets the right care in the right place at the right time.
Increasing flexibility and circularity through service business models
Healthcare organizations are increasingly implementing ‘as a service’ business models. For example, many are turning to SaaS (Software as a Service), whereby cloud-based systems give physicians, staff and even patients the opportunity to access data remotely, share critical insights in real time and collaborate more effectively, for better care coordination. SaaS models generally require a lower initial investment, and give organizations the financial flexibility to ’pay as they go,’ leading to more predictable costs.
Another benefit of SaaS models is their overall energy efficiency. When companies move to the cloud, their average server utilization can approach 65% compared with just ~15% on-premise. And while the PUE (Power Usage Effectiveness) of the average data center is 1.7, the cloud industry average is just 1.2. In short, this means fewer servers are required, and that any servers that are in use are consuming less energy.
Decarbonizing healthcare through renewable energy and efficiency
The healthcare sector is a major source of greenhouse gas emissions, accounting for over 4% of global CO₂ emissions. Health leaders across the world recognize the health implications of climate change – and the industry’s responsibility to take action.
The greatest scope for improvement lies in the transition to renewable energy, as well as in improving the lifetime energy efficiency of the devices and systems used in healthcare. Electricity consumption while in use accounts for the vast majority of these products’ total environmental impact. On a global level, it is primarily the combined effect of renewable energy and energy efficiency that will drive decarbonization.
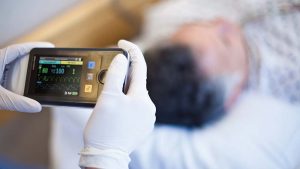
Photo Credits: Philips
Helping health consumers make sustainable choices through eco-labeling
In the rapidly expanding world of e-commerce, it is not unusual for consumers – including those buying personal health devices – to buy the same product in two or three formats to try them out at home. According to Pitney Bowes, 51% of shoppers consciously overbuy online, knowing they’ll return the items they don’t want. But when it comes to returns, too often, somewhere in the chain, it ‘pays’ to destroy the product and avoid the costs of transport, storage, relabeling, etc., rather than going back to the source.
Highlight the environmental benefits of ‘rethinking returns’ through better-informed ordering. In Europe, we see more and more brands signing up to the EU’s Green Consumption Pledge to raise awareness of products’ environmental footprint. One way they can do this is through the adoption of eco-labeling.
Turning innovations and commitments into measurable outcomes
Being able to measure and report outcomes in granular detail is central to proving the value of healthcare services, helps providers compare treatment options, and reveals opportunities for improving or even redefining care. Providing granular outcome data is increasingly becoming a requirement for unlocking reimbursement pathways, as the healthcare industry transitions away from fee-for-service models and towards value-based care.
As pressure mounts for healthcare companies to step up their actions to safeguard the health of people and the planet, there is an increased demand for proven results. This is why healthcare organizations are putting more resources into measuring not just clinical outcomes, but outcomes relating to social impact and environmental sustainability, too – such as proof of carbon-neutrality, or use of renewable energy sources.








